Keloid Scars
Last updated on October 2nd, 2023
What is keloid?
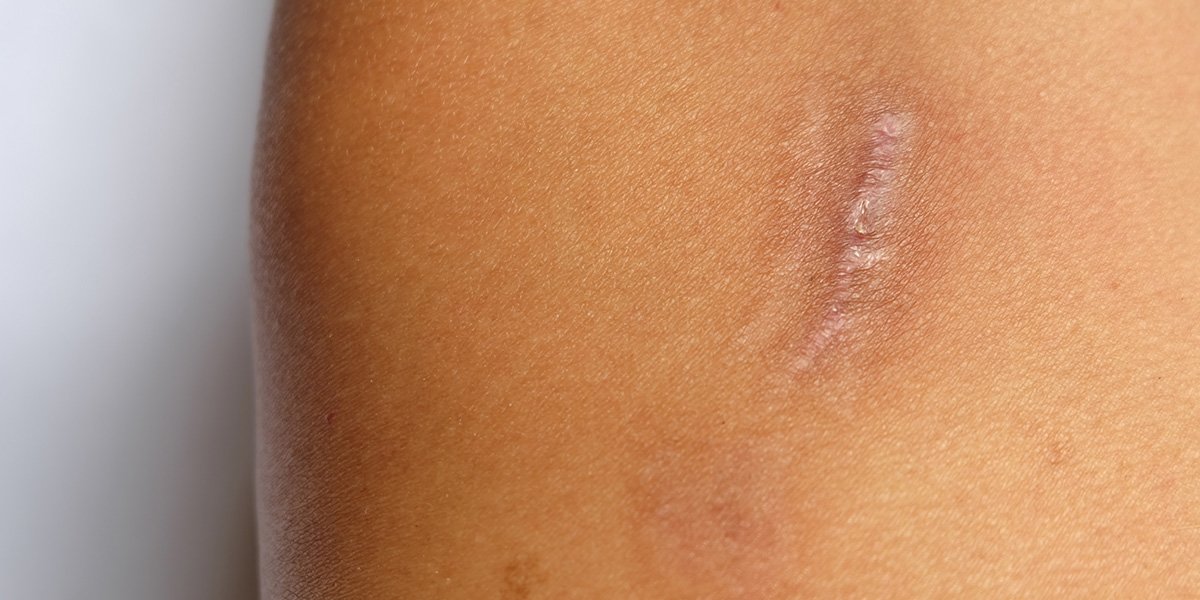
Keloids are larger and more pronounced than regular scars. They can be painful or itchy, and may also pucker. They extend beyond the edges of an original wound or incision. A keloid scar is sometimes confused with a hypertrophic scar. However, keloid usually grows beyond the borders of the original wound whereas in a hypertrophic scar the tissue stays within the wound border.Keloids can occur anywhere on the body, but they develop more commonly where there is little underlying fatty tissue, such as on the face, neck, ears, chest or shoulders. Keloid generally develops around a wound. The cause is unknown but it’s more common in people with darker pigmentation. It can develop after acne spots and boils, body piercings, burns, lacerations and surgical wounds. Infection increases the risk. There seems to be a problem with cells called fibroblasts which are responsible for the production of scar tissue (collagen). It is not know whether there is something wrong with the fibroblasts themselves or whether there is a problem with the chemicals which control their activity. Hormones, genetic factors and problems with the immune system have all been suspected of being involved. treatments are available. People prone to develop keloid should avoid piercings, tattoos and unnecessary surgery.
Who gets keloid?
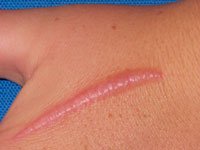 Keloid scars are more common in people with darker skins, especially African-American races. Average age is 10-30 years and keloids are less common at beginning of life or end of life. There is evidence that a family history of keloid plays a part in an individual developing keloid.
Keloid scars are more common in people with darker skins, especially African-American races. Average age is 10-30 years and keloids are less common at beginning of life or end of life. There is evidence that a family history of keloid plays a part in an individual developing keloid.
What are the symptoms of keloid?
Keloid typically starts to develop about three months after the original skin damage although it can take up to a year. A rubbery scar tissue starts presenting beyond the borders of the original damage. It may become tender, itchy, painful or produce a burning sensation. Sometimes keloid develops without any apparent skin injury. The common areas are the breastbone, shoulder, earlobe and cheek. Keloid growing over a joint can restrict movement. Over time, the red color changes to brown or becomes pale.
What is the treatment for keloid?
A keloid scar may shrink over time but rarely disappears completely. To reduce the appearance of keloid, a myriad of treatments can be effective. Treatment types are steroids, surgery, occlusive dressings, radiotherapy, cryotherapy, laser treatment, interferon treatment, cytotoxic drugs and micro-needling. Each of these treatments carries with it risks and side effects. The modality with the least risk and side effects, compared to the other methods listed, would be micro-needling. To find an authorized Dermapen Practitioner, please visit Skin Evaluation.
Find certified Dermapen microneedling professionals
Dermapen® Microneedling Devices are exclusively sold to Medical and Skin Care Professionals. Use the form to the right to get started finding a Certified Dermapen® practitioner in your area.
Enter your location information to find a Dermapen Skin Care Professional.
Want to become a Dermapen Practitioner?
Medical Clinics and Spas can offer their patients the worlds most advanced microneedling treatments with Dermapen
Microneedling Treatments
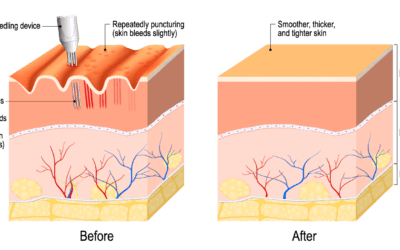
The Dermapen Microneedling Pen provides an unparalleled response through the segmented delivery of microneedles, creating micro injuries to the epidermis (outer layer of skin) and dermis (the inner layer of skin). As a result, the micro injuries encourage the body’s innate ability to repair itself.
Every Dermapen tip is outfitted with 12 needles and features our patented technologies, which include SureSpace™ and SafLok™. Accordingly, these safety enhancements can be found in every Dermapen needle tip and pen.
Furthermore, by using SureSpace™ and SafLok™ microneedling pen technologies, practitioners can deliver their patients the safest microneedling treatment possible, while getting the best microneedling results for their patients.