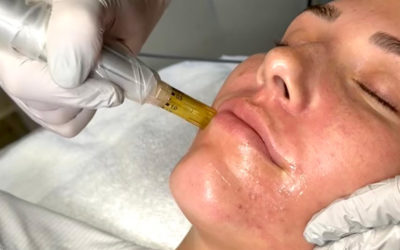
Micro Needle Dermabrasion
Last updated on September 17th, 2019

Microdermabrasion, or abrasive removal of epidermal tissue for therapeutic ends, has numerous applications and has long been a less aggressive alternative to indications treatable by laser- or other energy-based therapies.[Karimipour 2010] In terms of the microneedle realm, microneedle dermabrasion (also known as percutaneous collagen induction, or PCI) could be simply defined as causing thousands of microscopic columns of epidermal damage via microneedle with the goal of stimulating neocollagenesis (among other benefits) for therapeutic effect, leaving the majority of the skin intact with only temporary compromise of barrier function. Although (like microdermabrasion) most often used for overall skin rejuvenation and treatment of aging skin or photodamage, other applications include treatment of acne scars and other types of scarring, thin or crepey skin, mild pigmentation issues, skin laxity, and other indications requiring basic collagen revision at their foundation.[Fernandes 2005]
Microneedle dermabrasion owes its origins to early use of needle therapy throughout recorded history, but its emergence as a modern modality began with Orentreich in 1995[Orentreich 1995] using a tri-beveled for dermal subcision of depressed scars. In 1996 Fernandes used a small round stamp with embedded needles for skin rejuvenation, followed by Camirand using tattoo needles to revise scarring in 1997.[Camirand 1997] From there the dermal roller was developed by Horst Liebl in 2000, and since then the safety and efficacy of microneedle dermabrasion and PCI are well demonstrated in the literature. Treatment of various indications in patient populations running the gamut of skin type has been reported.
By creating fractional patterns of microscopic wounds—leaving the majority of local tissue undamaged—the wound healing cascade is triggered in the entire treatment area with minimal and rapidly-resolved compromise to the dermal barrier. Growth factors flood the area and upregulate fibroblast production and activity, which in turn stimulate keratinocyte proliferation and action. Microneedling was shown in a 2010 study by Aust and colleagues [Aust 2010] to upregulate the expression of specific transforming growth factors in rats over a two week period post-procedure; the growth factors in question promote healthy, scar-free wound healing. The production of a base of healthy new collagen is the result, a process which continues over the course of months, creating healthier skin with increases in thickness as well. [Fernandes 2005] There is also hypothesized additional microelectrical stimulation of the healing cascade as well, due to the nature of microneedle penetration.
Advantages to microneedle dermabrasion with Dermapen are numerous. Treatment itself is inexpensive, easy to perform, and relatively painless in comparison to most alternatives. Simplicity and tolerability of treatment contribute to rapid treatment speed; little in the way of pre- or post-procedure protocol is required, and treatment time low. Rapid vertical insertion of microneedles is minimally traumatic. The nature of microneedle treatment makes it possible on almost any body area, which is not true for competing modalities. The use of disposable treatment tips maximizes sterility. Brief compromise of barrier function means healing is rapid; adjunctive use of topicals may play also a greater role via improved penetration through the temporary microchannels created during therapy.
Additionally, the therapeutic epidermal damage caused by microneedle dermabrasion results in apoptosis (programmed cell death) rather than necrosis which is associated with many popular skin rejuvenation alternatives such as laser-based modalities.[Ziegler 2004] Necrosis causes unwanted maintenance of the inflammatory cascade which may increase the risk of post-inflammatory hyperpigmentation (PIH), especially in darker-skinned populations prone to the condition.[Chan 2007] Dermal rolling was used in rats in a 2008 controlled study [Aust 2008] examining incidence of post-treatment dyspigmentation; data suggested no evidence that microneedle therapy induced dyspigmentation, and in fact expression of key markers of melanocyte stimulation were slightly inhibited.
Microneedling is useful all over the body as well. For example, a 2010 pilot study abstract [Aust Viewpoints 2010] explained the similarities between the skin characteristics of the aging face versus aging hand as a rationale for treating the dorsal hands of three patients (aged 52 to 61 years) using a dermal roller for 20 to 30 minutes at different vectors. Improvements in skin texture, tightening, and vascularization were noted.
needle dermabrasion needle dermabrasion or needle abrasion or dermabrasion treatment or mechanical dermabrasion with Dermapen.
Find certified Dermapen microneedling professionals
Dermapen® Microneedling Devices are exclusively sold to Medical and Skin Care Professionals. Use the form to the right to get started finding a Certified Dermapen® practitioner in your area.
Enter your location information to find a Dermapen Skin Care Professional.
Want to become a Dermapen Practitioner?
Medical Clinics and Spas can offer their patients the worlds most advanced microneedling treatments with Dermapen
Microneedling Treatments
The Dermapen Microneedling Pen provides an unparalleled response through the segmented delivery of microneedles, creating micro injuries to the epidermis (outer layer of skin) and dermis (the inner layer of skin). As a result, the micro injuries encourage the body’s innate ability to repair itself.
Every Dermapen tip is outfitted with 12 needles and features our patented technologies, which include SureSpace™ and SafLok™. Accordingly, these safety enhancements can be found in every Dermapen needle tip and pen.
Furthermore, by using SureSpace™ and SafLok™ microneedling pen technologies, practitioners can deliver their patients the safest microneedling treatment possible, while getting the best microneedling results for their patients.