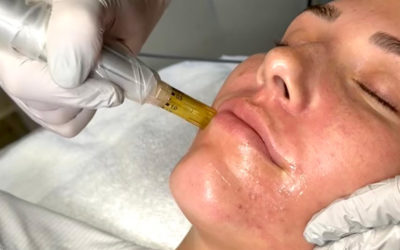
Dermapen For Acne Scars
Last updated on September 17th, 2019

Acne is a common skin condition among teens with possible extension into or onset during adulthood. The active disease may affect quality of life, but it is sequelae such as scarring that seem to be the culprit behind most negative emotional impact associated with the condition. Thus, treatment of acne scarring is a prime concern of dermatologists and any physician working in the aesthetic realm.
Percutaneous collagen induction (PCI) via dermal roller microneedling has been shown in the literature to be an effective method for treating acne scars, especially rolling scars, superficial boxcar scars, and low grade macular scars, in the same vein as laser fractional resurfacing.[Fabbrocini 2010] By creating thousands of minute but relatively shallow holes in the stratum corneum and leaving the majority of local tissue undamaged, the wound healing cascade is triggered and upregulated in the entire treatment area with minimal and rapidly-resolved compromise to the dermal barrier. Growth factors flood the area and stimulate fibroblast production and activity; keratinocyte proliferation and action follows soon after. The production of a base of healthy new collagen is the result, a process which continues for months, building up healthy skin and volume within scarred areas.
A presentation from a medical conference in Australia compared dermal rollers directly with Dermapen in 60 patients with atrophic acne scarring, a confrontation in which Dermapen was demonstrated to be superior in all ways including outcomes, treatment comfort, and ease of use. [Chu 2012]
Patients with skin of color may be predisposed to acne just like those with lighter skin, but treating this subset of the population has posed a challenge to the medical community. Many successful treatments are laser-or-light based, which is problematic for patients with skin of color due to the increased concentrations of dermal and epidermal melanin, which causes more rapid build-up of heat. Also, with many therapies there is increased risk of development of keloid scarring or post-inflammatory hyperpigmentation (PIH) due to irritation from cutaneous physical and thermal trauma; therefore management of risk of PIH is an essential component to therapy.[Shah 2009] Dermapen is proven successful for acne scarring without use of light or laser. Additionally, trauma to skin is minimal with little irritation at the dermal/epidermal junction, so there is very little risk of PIH. Additionally, other methods may be more prone to inducing cellular necrosis (and associated stimulation of the inflammatory cascade) rather than apoptosis (programmed cell death) which does not contribute to over-inflammation.[Ziegler 2004]
A published study by Fabbrocini and colleagues [Fabbrocini 2009] examined microneedling (via standard dermal roller) for rolling acne scars in 32 patients (20 female, age range 17 to 45). Protocol included 3 weeks of topical therapy before microneedling. Analysis of digital photography and microrelief analysis of facial molding (n=5) revealed statistically significant reductions in severity of scarring after two sessions, with notable overall aesthetic improvement and no dyspigmentation side effects. The abstract of a 2010 study of percutaneous collagen induction for acne scarring by Fabbrocini [Fabbrocini 2010 abst] described the treatment of 60 acne scar patients (36 women, mean age 27 years, skin types I to VI). Each received three treatments at intervals of 4 to 12 weeks. Digital analysis of photopraphy showed significant aesthetic improvement with no incidence of dyspigmentation in even the darkest skin types.
Chu T. Treatment of atrophic acne scarring – Dermaroller vs Dermapen. Abstract presented at Cosmetex 2012, Cairns, Queensland, Australia.
Find certified Dermapen microneedling professionals
Dermapen® Microneedling Devices are exclusively sold to Medical and Skin Care Professionals. Use the form to the right to get started finding a Certified Dermapen® practitioner in your area.
Enter your location information to find a Dermapen Skin Care Professional.
Want to become a Dermapen Practitioner?
Medical Clinics and Spas can offer their patients the worlds most advanced microneedling treatments with Dermapen
Microneedling Treatments
The Dermapen Microneedling Pen provides an unparalleled response through the segmented delivery of microneedles, creating micro injuries to the epidermis (outer layer of skin) and dermis (the inner layer of skin). As a result, the micro injuries encourage the body’s innate ability to repair itself.
Every Dermapen tip is outfitted with 12 needles and features our patented technologies, which include SureSpace™ and SafLok™. Accordingly, these safety enhancements can be found in every Dermapen needle tip and pen.
Furthermore, by using SureSpace™ and SafLok™ microneedling pen technologies, practitioners can deliver their patients the safest microneedling treatment possible, while getting the best microneedling results for their patients.