Fractional Dermabrasion vs Fractional Laser Therapy
Last updated on May 16th, 2022

Most aesthetic medical devices operate on the principle that controlled wounding of skin and underlying tissue will cause a healing response, stimulating neocollagenesis and the creation of healthier-looking skin. Fractional laser therapy is the controlled creation of patterns of microscopic wounds in the skin via laser, each surrounded by islands of healthy tissue from which relatively rapid re-epithelialization and healing can begin. Light energy is converted to heat resulting in the coagulation of proteins and, depending on the device, ablative damage as well. Collagen growth is stimulated and over time a marked increase in collagen is seen.[Gold 2010] Inflammation is an unfortunate side effect, and post-inflammatory hyperpigmentation may result in some cases.[Chan 2007, Metelitsa 2010] The technology was developed in response to a reduction in the popularity of the ablative CO2 laser which, although the gold standard for a variety of indications such as scar revision and reduction of fine lines and wrinkles at the time, was plagued by a weakening reputation for long downtime and risk of side effects, especially pigmentation problems. With fractional therapies results were less dramatic but downtime and risk were markedly reduced. Since its inception in 2004, the technology has been further refined to produce even better outcomes.[Gold 2010]
There is a wide variety of fractional laser devices on the market and they differ in a variety of ways, most notably in the wavelength employed in the device and the scanning technology. Wavelength accounts for the way laser energy affects the skin and the character of each wound; the diameter and depth of each microwound, as well as any collateral thermal damage seen in surrounding tissue, are key factors that depend on the absorption spectrum of each wavelength. The scanning technology determines the pattern, speed, and order of the creation of each wound in a treatment spot; the purpose of modulating those factors is to control unwanted buildup of heat which may affect treatment comfort or the quality of the outcome. As such, devices employing different wavelengths and scanning technology will be better for different indications.[Gold 2010] Wound character can also be modulated by varying the level of energy delivered and the space between each microwound. Recently, the list and incidence of potential complications has been widened to range More recent review of the modality in the literature suggests that the incidence and variety of complications is greater than previously thought, ranging from mild (prolonged erythema, acne) to severe (hypertrophic scarring, disseminated infection).[Metelitsa 2010]
Despite its popularity, fractional laser therapy is a technically complicated way of doing what can be achieved simply with Dermapen. The proper use of each device demands a high level of education, training, and experience. Users must understand how and why to adjust various treatment parameters depending on the indication as well as the patient’s individual characteristics. For patients with darker skin, especially Asians, use of lasers is problematic due to the high levels of melanin as a competing chromophore and the increased potential for side effects, especially post-inflammatory hyperpigmentation (PIH).[Chan 2007] Mistakes can be life-altering.
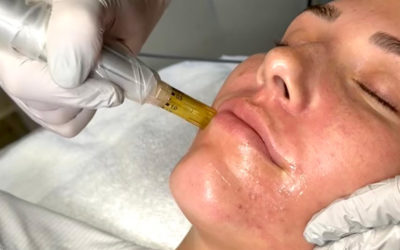
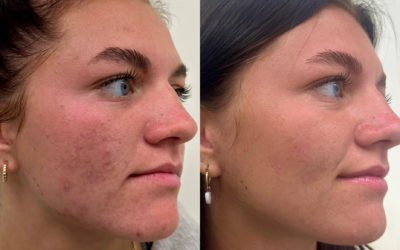
Percutaneous collagen induction (PCI) can be viewed as a simple alternative to fractional laser therapy. [Fernandes 2002] In essence, fractional microneedle therapy with Dermapen is similar to fractional laser therapy in that it creates patterns of tiny wounds, controlled trauma to tissue meant to stimulate neocollagenesis and cause tissue remodeling via the body’s natural wound healing response. The difference is that controlled damage caused by the vertical puncture with surgical steel microneedles leads to apoptosis (programmed cell death) rather than ablation or coagulation via thermal insult, which leads to necrosis. Histological study has shown apoptosis to be a more regulated process; the controlled, staged cell death is almost completely free of excess inflammation because cell membranes remain intact for a relatively long time. Necrosis is more chaotic and usually results in a much greater degree of inflammation. [Ziegler 2004] The inflammatory cascade is part of the mechanism behind heightened risk of PIH, hence the lack of PIH seen with Dermapen therapy. In fact, a major advantage of PCI is that its gentler approach lends it to repeat treatment. [Fernandes 2002]
Depth of damage is controlled by choice of microneedle length. The spacing of wounds or order in which they are created doesn’t matter, because collateral thermal damage or treatment discomfort due to heat buildup is not an issue. Skin color is not a factor in treatment the way it is with any laser therapy. And while marked increase in collagen is seen with Dermapen therapy, inflammation is minimal, thus side effects are minimal and safety is greater. Additionally, the simplicity and safety of Dermapen microneedle therapy make it easy to delegate to ancillary staff with confidence.
Find certified Dermapen microneedling professionals
Dermapen® Microneedling Devices are exclusively sold to Medical and Skin Care Professionals. Use the form to the right to get started finding a Certified Dermapen® practitioner in your area.
Enter your location information to find a Dermapen Skin Care Professional.
Error: Contact form not found.
Want to become a Dermapen Practitioner?
Medical Clinics and Spas can offer their patients the worlds most advanced microneedling treatments with Dermapen
Microneedling Treatments
The Dermapen Microneedling Pen provides an unparalleled response through the segmented delivery of microneedles, creating micro injuries to the epidermis (outer layer of skin) and dermis (the inner layer of skin). As a result, the micro injuries encourage the body’s innate ability to repair itself.
Every Dermapen tip is outfitted with 12 needles and features our patented technologies, which include SureSpace™ and SafLok™. Accordingly, these safety enhancements can be found in every Dermapen needle tip and pen.
Furthermore, by using SureSpace™ and SafLok™ microneedling pen technologies, practitioners can deliver their patients the safest microneedling treatment possible, while getting the best microneedling results for their patients.